Drugs and Diagnostics
Drug-based strategies for malaria control and elimination
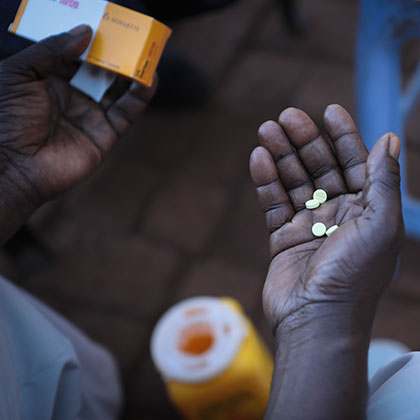
Antimalarial drugs are essential for both treatment and prevention in malaria control and elimination programs. All countries with endemic malaria use drugs for clinical case management, where antimalarial medicines are used to treat confirmed clinical cases of malaria. Beyond clinical case management, drugs can be used to prevent and treat malaria among specific at-risk populations. These uses are referred to as chemoprevention strategies and can be used to reduce malaria transmission and morbidity, and respond to emergencies including malaria outbreaks or situations where the health system is strained (e.g., during an Ebola outbreak).
When implementing a chemoprevention strategy, there are numerous options to choose from depending on programmatic objectives, local contexts, resources available, and specific transmission dynamics. Strategies include improving access to treatment for malaria with an efficacious drug, intermittent-treatment programs, and mass drug administration, with and without first screening for malaria. In particular, drug-based strategies to reduce transmission of malaria need to target the asymptomatic carriers of infection, including high-risk populations. However, there are limited studies that have assessed this challenge and its implications. The MEI conducts trials and reviews to assess the effectiveness of various drug-based strategies to reduce or interrupt malaria transmission. The MEI also develops tools to guide decision-making on the use of drug-based strategies for elimination. These have included a tool for mass drug administration and screen and treat strategies, and pharmacovigilance of single dose primaquine. Currently, the MEI is developing a risk-benefit assessment tool regarding treatment regimens against Plasmodium vivax.
Diagnostics for passive and active case detection
Accurate diagnosis of malaria is critical for appropriate patient management and population-level surveillance. While standard diagnostics such as microscopy and rapid diagnostic testing (RDTs) are generally considered to have reliable accuracy, the changing epidemiology of malaria in low-transmission settings presents new challenges. Specifically, a higher proportion of infections in these settings are below the reliable detection limit of RDTs and microscopy.
The MEI conducts research to assess the effectiveness of existing diagnostics in low transmission settings and the factors that influence the accuracy of these tests when used for passive and active case detection for surveillance. The MEI also conducts research to understand the role of novel detection methods including highly sensitive molecular methods, serologic methods, and more sensitive rapid tests. More recently, the MEI has been engaged in research on new point-of-care tests for glucose-6-phosphate dehydrogenase (G6PD) deficiency, an X-linked trait that can cause some individuals to be at risk of hemolytic toxicity following treatment with the antimalarial primaquine.